
Cross-posted from The Conversation:
There is an old joke about one fish asking another about the state of the water and the other answering “what’s water?” When you’re immersed in something and that is your daily experience, you are not able to step outside it – all you see is what you know.
But with all the talk about Australia’s health system being unsustainable, it’s useful to step back and look at the Australian health system in an international context.
So, how do we perform against our peers? The short answer is pretty well.
Comparing inputs and outcomes
Much of the sustainability talk is about costs, and only about costs. Costs are important, but any reasonable comparison of Australia’s standing also takes into account what we get for the spending. Measuring costs is (relatively) easy. We can compare cost per head spent on health care (standardised across countries into a common monetary unit) or costs as a share of gross domestic product (GDP).
Measuring the benefit side is a bit trickier. The most common comparisons of outcomes are mortality-based measures, partly because measurement is definitive. There are choices here too. Life expectancy and a measure of “early deaths” (deaths before age 70) known as “potential years of life lost” are the two most common.
Using these mortality-based measures to compare health systems has a number of weaknesses. It assumes that the most important contribution of the health system is delaying death, ignoring quality of life. They also assume that the health system is the most important contributor to life expectancy, ignoring broader socioeconomic and environmental factors such as clean water, employment and good nutrition.
Despite these weaknesses, the measures are commonly used, readily available for comparable countries and they’re the best we’ve got.
Better than average
The graph below shows where Australia sits compared to similar OECD countries (countries within 25% of Australian GDP). Countries which are better than the OECD average on life expectancy are on the right hand side. Countries that spend a smaller share of GDP on health care are on the lower part of the graph.
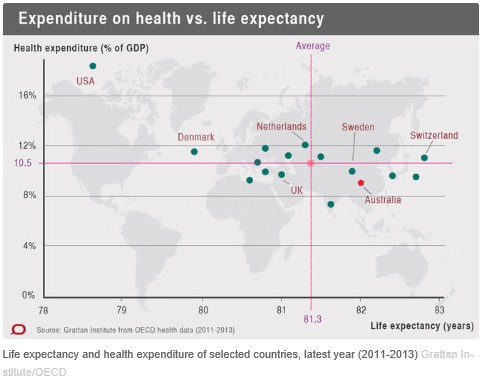
Australia is in the good quadrant: better than average life expectancy, lower than average share of GDP. The stand-out poor-performing country is the United States, with high costs and poor outcomes.
So we’re OK now, but are we going downhill?
The graph above shows data for the most recent year available. Australia’s historic trends are also good. In 2001, Australia spent 8.2% of GDP on health; ten years later GDP share had increased to 9.1%. Over the same period, the comparable country average had increased faster – from 8.8% to 10.3%.
Our life expectancy improvements essentially mirrored other comparable countries.
This suggests that in addition to being in a good position now, the trend in both inputs and outcomes over the past decade has been a healthy one, comparably.
No cause to be complacent
Australia is performing well against our peers, and has done so over the past few decades. But current life expectancy is the product of past policies. And past good performance doesn’t guarantee we are well positioned for changing health-care needs.
Equity concerns
It’s important to remember that the data above are country averages. In Australia’s case, the average masks very poor performance for our Indigenous populations whose average life expectancy is around ten years shorter than non-Indigenous Australians. Poorer Australians also have worse health outcomes.
There are other equity issues as well. A Grattan Institute submission to a recent Senate Committee inquiry showed that some households face very high levels of out-of-pocket costs. Australian Bureau of Statistics surveys show people are already deferring care because of high out-of-pocket costs.
Access to care for people in rural and remote Australia is much worse than in metropolitan areas, causing problems not only in term of health status but also in increased cost of care.
Future care needs
Repositioning the health system to address the challenges of chronic disease is hard. It seems obvious that a system that pays doctors for seeing patients again and again is probably not suitable to encourage continuity of care and looking after a person for an ongoing illness.
Unfortunately, getting beyond that simplistic statement is complex. The evidence on the best way to pay doctors is quite weak and so moving forward on better payment systems will require experimentation to identify what works in the Australian context.
Structural changes, to improve seamlessness of care to ensure that a person with chronic illnesses has access to all the professional skills needed, will also be required.
Prune waste
Science advances, and with it come new treatments and new demands for funding. The increasing prevalence of chronic illness creates another set of pressures on health spending.
There are a number of potential responses to the challenge of increased costs. The worst is to panic and adopt draconian “quick fixes” which aren’t fixes at all. The $7 co-payment proposal, which shifts costs rather than saves them, is an example of this approach.
The alternate pathway is to attack waste in the health system: there are inefficiencies in hospitals, in the way we use our highly skilled health professionals and in how we pay for pharmaceuticals. Billions of dollars can be freed up in these areas.
Pruning waste is hard as every dollar of health spending is a dollar of someone’s income, profits or revenue. Rent seekers will be out in force to defend the status quo. Paraphrasing another famous saying, political leadership was never meant to be easy but nevertheless, Operation Eliminate Healthcare Waste should surely be a political priority.
Where to from here?
Australia is not alone in facing these challenges: the changing health-care profile is a universal phenomenon. Other countries are addressing these issues and we can potentially learn from those experiences. The Conversation will be publishing five “country studies” over the next week to explore these international lessons.
Article by Stephen Duckett, Director, Health Program at Grattan Institute

